Ventilation Standards for OPA, Glutaraldehyde, and Hydrogen Peroxide

Customers regularly ask us specific questions about vapor and fume control, which has been our area of expertise since 1995. That said, this week's blog is dedicated to fume and ventilation standards associated with high-level disinfectants.
Overview: All high-level disinfectants, including glutaraldehyde, OPA, and hydrogen peroxide, are designed to kill microorganisms, and have the potential to be irritants and possibly sensitizers.
What are the ventilation standards regarding high-level disinfectants & vapor control?
ANSI published a set of standards in 2005 entitled, "Chemical Sterilization and High-level Disinfection in Health Care Facilities." The section dedicated to ventilation states1:
- Chemical sterilants should be used in an area that is properly ventilated.
- Rooms in which chemical disinfection and sterilization are performed should have a minimum of 10 air exchanges per hour (local regulations may require a higher minimum exchange rate).
- When general room ventilation is not adequate, a self-contained, freestanding system* or a local exhaust hood should be installed to capture chemical vapor during processing.
- When an outside exhaust system is not available, a ductless fume hood* can be used to deliver vapor to a filter system that chemically inactivates the vapor; then clean, filtered air is returned to the room.
- Filters for these systems should be replaced at regular intervals.
*A ductless fume hood is simply a freestanding system that captures the toxic fumes and vapors and returns clean air to the room. Other names for ductless fume hoods are vapor control systems and disinfection soak stations.
The Joint Commission and OSHA look to see that health care facilities protect workers and patients from known risks. Since all high-level disinfectants by definition are toxic, and their fumes are known irritants, workers and patients need protection from exposure. Proper handling and use of high-level disinfectants falls under The Joint Commission's Environment of Care Standards:
EC.02.02.01:The hospital minimizes risks associated with selecting, handling storing, transporting, using and disposing hazardous gases and vapors.2
Three Commonly Used High-Level Disinfectants:
1. OPA (Ortho-Phthalaldehyde):
Since OPA's introduction to the market in 1999, it has emerged as one of the most popular high-level disinfectants in the industry. It is mostly odorless and has a 12-minute disinfection soak time.
- CIDEX OPA's MSDS states that the disinfectant should be used "in a well-ventilated area and used with the appropriate exhaust ventilation, for example, a minimum of 10 air exchanges per hour."
- CIDEX OPA's Instructions for Use recommend a 'ductless fume hood' or 'portable ventilation device' if adequate ventilation is not provided. As previously stated, these terms are synonymous with a disinfection soak station or a vapor control system.
2. Glutaraldehyde:
Glutaraldehyde was the most common high-level disinfectant for several decades. There are numerous brands with varying features (activation, shelf life, etc.). Glutaraldehyde has a pungent odor and the disinfection soak time ranges from 20 to 45 minutes at 77°F.
OSHA has a current exposure level limit of 0.2ppm and ACGIH has a lower exposure limit of 0.05ppm. The engineering controls are virtually the same for OPA and glutaraldehyde: 10 air exchanges per hour.
3. Hydrogen Peroxide:
Hydrogen Peroxide is a newer high-level disinfectant with a disinfection soak time of only 8 minutes at 68°F. A benefit of hydrogen peroxide is that it requires only one low volume rinse (verses 3 large volume rinses of 1 minute each for OPA).
A minimum of 6 air changes is required when working with hydrogen peroxide, such as UltrOx™. In some areas, such as the soil room, 10 air changes is required. The safety sheet for UltrOx™ indicates that the ACGIH TLV and OSHA PEL is 1 ppm. The CDC’s guide on hydrogen peroxide states that exposure routes can derive from inhalation, ingestions, skin and/or eye contact.
Like OPA and glutaraldehyde, hydrogen peroxide is a high-level disinfectant that kills microorganisms. Although it is not an aldehyde, all chemicals should be respected for their potency - they are all chemicals that can be harmful.
What is an Air Change?
A single air change is the total volume of air in a room being replaced every hour. If you're working with a disinfectant that requires 6 air changes, then the total volume of air (all of the air) in that given workspace has to be completely replaced with fresh air 6 separate times in one hour. In reality, this guideline is rarely met, particularly in older buildings or ones that have been renovated.
In order to determine the amount of air that is entering the room from the HVAC, you would use a specialized capture hood. Most hospitals will have one in their Biomed or Maintenance departments.
Do you still need vapor control if you have at least 6-10 air changes per hour?
In many cases, yes, because air exchanges don't necessarily solve the issues with air flow patterns in your work space.
- Most rooms have the supply and return vents (for air-conditioning & heating) in the ceiling. This often results in the air 'short circuiting' and taking the quickest route, going from the supply vent directly to the return vent. So even though there may be a minimum of 6-10 air exchanges, the air is not being properly mixed in the breathing zone. (See figure below)
- In some cases when the return air vent is located above the soaking container, it will actually draw the fumes up into the breathing zone. (See figure below)
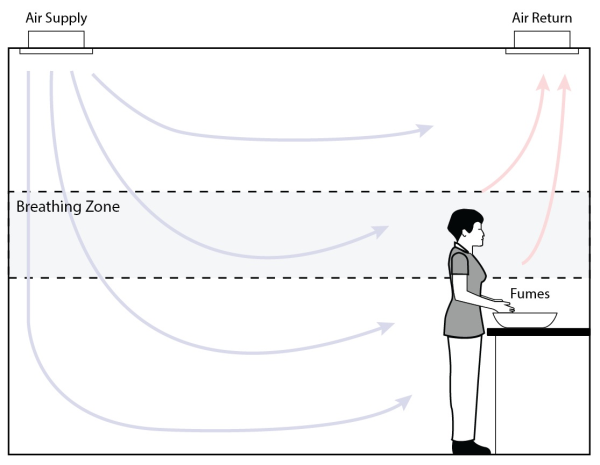
Important to Note: The above scenarios address manual soak disinfection. Automated reprocessors also can exceed exposure level limits when high-level disinfectants are poured into the reservoir or when the process is stopped mid-cycle.
References
- Chemical Sterilization and high-level disinfection in health care facilities. ANSI/AAMI (American National Standards Institute) ST58:2005. Section 3.4: Ventilation of Processing Areas and Equipment
- 2009 CSR TJC Hospital Accreditation Standards, EC.02.02.01, Section 9
- Guidelines for Environmental Infection Control in Health-Care Facilities, 2003






